By Muhammad Irfan
The AstraZeneca shot was recently open to the public for registration on 2 May and was fully booked within four hours. Although the support by Malaysians for herd immunity can be seen through this, a handful of Malaysians are still hesitant to take the AstraZeneca shot.
The issue which arises among doubtful Malaysians to take the AstraZeneca vaccine are stemmed by two reasons.
The first reason is the risks that come with the AstraZeneca shot. It is reported by the European Medicines Agency (EMA) that blood clots could happen in people who received the AstraZeneca shot. EMA also reported that the AstraZeneca shot could cause low blood platelets which assists in blood clots.
However, according to the Medicines & Healthcare products Regulatory Agency (MHRA), the chances of blood clots to happen after receiving the AstraZeneca shot is very low. It is documented by the MHRA that the risk for serious blood clots to happen is 0.0004% or 4 people in every 1 million people.

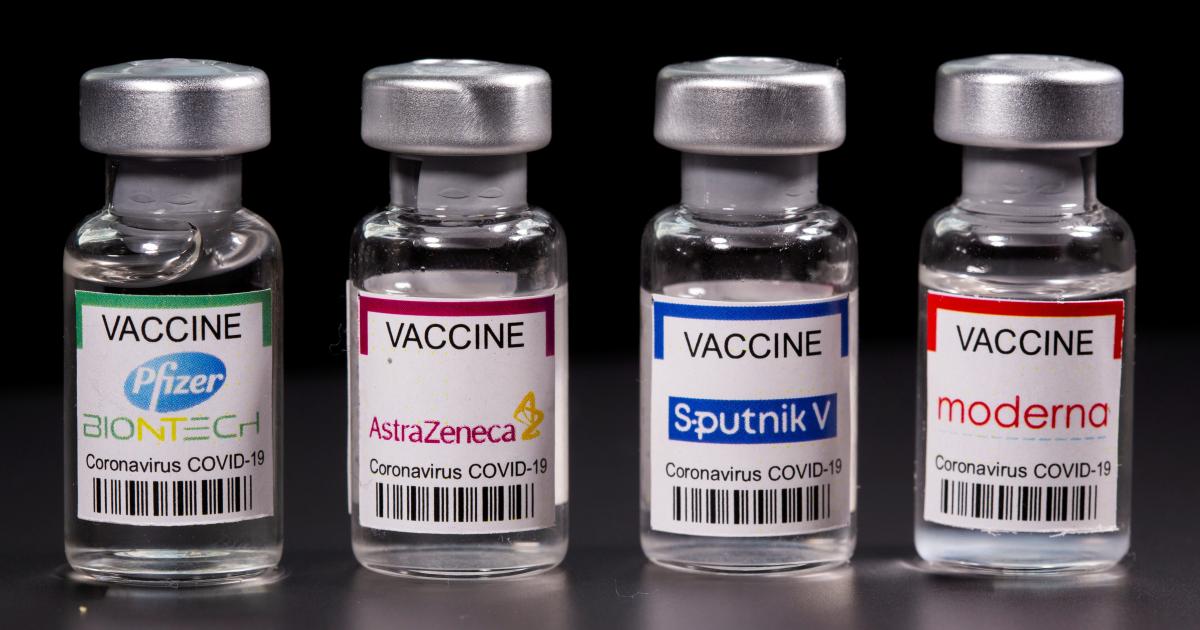
The second reason that makes Malaysians hesitant to take the AstraZeneca shot is due to its low efficacy rate when compared with other vaccines. According to the national Covid-19 immunisation programme portfolio, the Malaysian government has acquired Covid-19 vaccines supply from four pharmaceutical companies and one research institute with different efficacy rates. The vaccines are commonly known as Pfizer, AstraZeneca, Sinovac, CanSinoBio and Sputnik V.
The Special Committee for Ensuring Access to Covid-19 Vaccine Supply (JKJAV) reported that the efficacy rate of Pfizer vaccines is 95% while AstraZeneca vaccines have an efficacy rate ranging between 62%-90%. The Sinovac vaccines have an efficacy rate range of 50.4% – 91.25% and CanSinoBio efficacy rate is 65.7% while Sputnik V is 91.6%.

From the report made by JKJAV, a person would tend to argue that Pfizer is the best vaccine. However, that is not the case. The efficacy rate of a vaccine does not determine whether one is more effective than the other.
To explain this, it is crucial for people to understand the process of how vaccines are clinically tested and the circumstances where the vaccines are clinically tested before the vaccines producers get their efficacy rates.
Vaccines are clinically tested on large trials with thousands of participants that are split into two groups. One group received a placebo while the other group received the vaccine. They are monitored by scientists for a few months to see if they develop Covid-19 after the vaccine and placebo shot.
The vaccine producers got the efficacy rates by analysing how many participants are diagnosed with Covid-19.
For example, a testing done by Pfizer had 43,000 participants and 170 of them were tested positive for Covid-19. The placement of the 170 participants, whether they are in the placebo or vaccine group determines the efficacy rate of the vaccine. In this specific testing, 162 people were from the placebo group while only 8 were from the vaccine group. Thus, the Pfizer vaccine has a 95% efficacy rate.
The term efficacy rate refers to the probability someone is unlikely to get Covid-19. For instance, Pfizer vaccines which have a 95% efficacy rate means that a person is 95% less likely to be diagnosed with Covid-19 rather than 5 people out of every 100 people who got the vaccine are diagnosed with Covid-19.
The circumstances where the vaccines are clinically tested to get the efficacy rates numbers also need to be taken into account to understand the difference of efficacy rates. To illustrate this, the Pfizer vaccine was developed primarily in the United States of America which have the original strain of Covid-19 and during times with a lower Covid-19 cases compared to the Sinovac vaccine which was developed in countries such as Brazil that has other variants of Covid-19. They also started testing later where Covid-19 cases were higher globally.
Thus, it can be deduced that the efficacy rates of the vaccines only recorded the occurrence during their clinical trials and not the real world as the world is changing day by day and new variants are found. This makes the efficacy rate not the best way to view a vaccine. Hence, it begs the question whether vaccines are even made to prevent Covid-19 infection.
A senior scholar from Johns Hopkins University Centre for Health Security, Amesh Adalja said œThe goal of a vaccine programme for Covid-19 is not necessarily to get to ˜Covid zero, but its to tame this virus, to defang it, to remove its ability to cause serious disease, hospitalization and death.
Therefore, it is understood that the vaccines are used to prevent people from developing severe symptoms, being hospitalized and dead rather than to stop the infection itself.
It is important to note that in all the vaccine clinical trials, none of the participants who received the vaccine was hospitalized nor died despite being infected with Covid-19. This proves that all the vaccines have an efficacy rate of 100% against death and hospitalization.
Hence, any vaccine regardless of its efficacy rate is reliable to avoid severe symptoms of Covid-19. This further enhances the need for people to get vaccinated in order to achieve herd immunity.
Consequently, it answers the question that no matter what vaccine people get, it will help them to stay alive, prevent hospitalization and eventually helps to end the pandemic.
As a researcher from University of Washington, Deborah Fuller said œThe best vaccine right now for you is the one youre offered.
To achieve herd immunity, Malaysians should register for the Covid-19 vaccination and book vaccination slots to whichever vaccine that is available at the time of offer. Covid-19 vaccination registration could be made through the MySejahtera application or through the JKJAV website.***